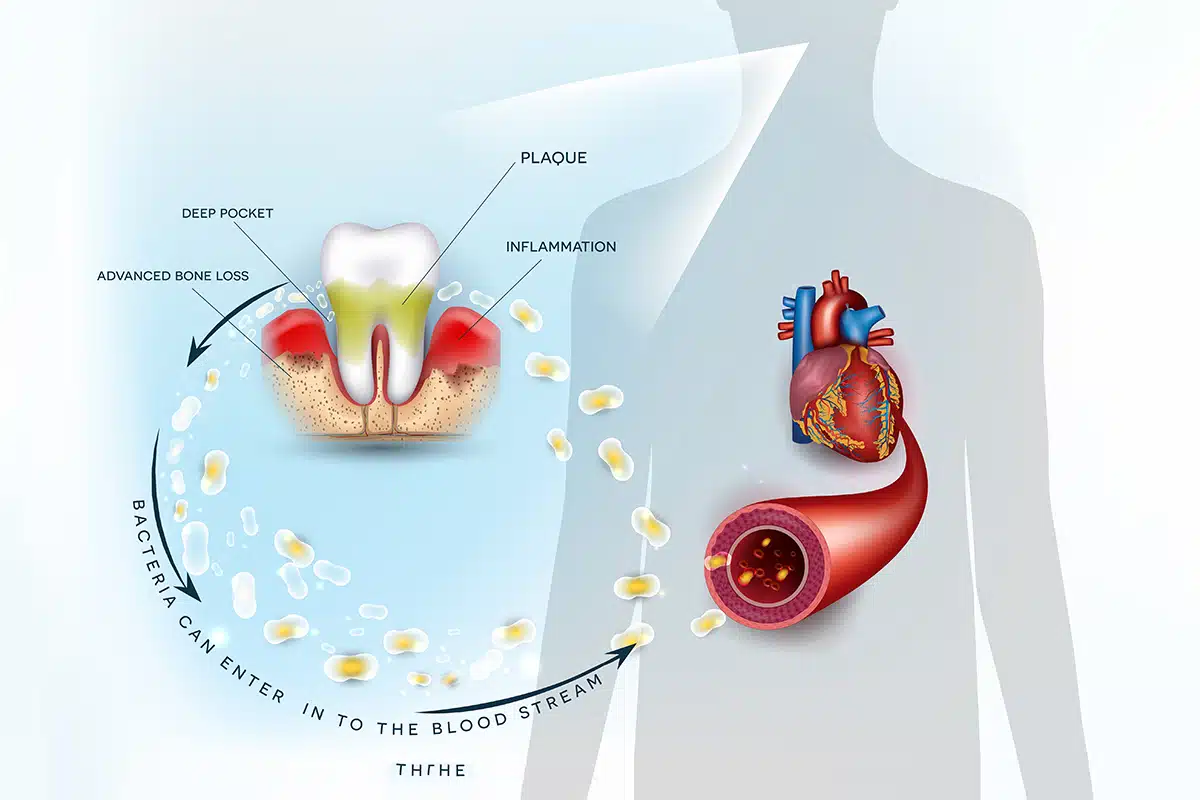
Have you ever brushed off a nagging toothache, assuming it would go away on its own? While dental pain might seem minor at first, ignoring it can lead to more than just a trip to the dentist. It can cause serious health problems that affect your entire body.
Infections that start in a tooth do not always stay localized. When bacteria spread beyond the mouth, they can reach other parts of the body and lead to complications such as sepsis, heart infections, or other serious conditions. Recognizing the risks early can help prevent the infection from becoming dangerous.
Can a Tooth Infection Affect Your Whole Body?
Yes, a tooth infection can spread beyond the mouth and affect the entire body. If left untreated, bacteria from the infection can enter the bloodstream, traveling to vital organs and potentially causing life-threatening conditions such as sepsis or endocarditis. This is why early diagnosis and prompt treatment are crucial, not only for saving your tooth but also for protecting your health overall. Understanding the symptoms of a spreading tooth infection can help you take action before it’s too late.
What Can a Tooth Infection Cause?
A tooth infection can lead to serious health problems if left untreated, especially when bacteria spread through the bloodstream to other parts of the body. These complications can range from localized infections to life-threatening conditions.
Common complications include:
- Sepsis: A life-threatening reaction to infection that can lead to organ failure
- Endocarditis: An infection of the inner lining of the heart and its valves
- Osteomyelitis: A serious bone infection that can affect the jaw or other areas
- Ludwig’s angina: Severe swelling in the neck and jaw that can block the airway
- Gum disease: Ongoing infection that damages the gums and supporting structures
- Dental cysts: Fluid-filled sacs that can develop near the infected tooth
Signs and Symptoms of Tooth Infection Spreading to the Body
When a tooth infection begins to spread beyond the root of the tooth, the body often sends out distress signals in the form of symptoms that shouldn’t be ignored. These signs can manifest subtly at first, but they may rapidly intensify as the infection moves through the bloodstream and into other systems.
Recognizing these symptoms early is crucial for preventing dangerous complications.
General Symptoms
As a tooth infection begins to spread beyond its original site, the body often responds with generalized symptoms that resemble those of the flu or a common illness. These signs are your body’s way of signaling that something more serious may be going on internally.
- Fever (above 101°F / 38.3°C) that lasts more than a day or spikes at night.
- Chills or shaking, where you feel cold and shivery even under blankets.
- Extreme fatigue or feeling “run‑down,” where normal daily tasks feel exhausting.
- Headache that doesn’t improve with rest and may get worse over hours or days.
- Muscle aches similar to those with a virus, but happening alongside a painful or swollen tooth.
Facial and Oral Symptoms
As the infection worsens, it often becomes more visible and painful in the face and mouth area. These symptoms can interfere with basic activities like eating, speaking, or even opening your mouth, and should be considered red flags for a spreading infection:
- Swelling of the face, cheek, or jaw that worsens over hours.
- Pain that spreads to the ear, jaw, or neck on the same side.
- Bad breath or bad taste that doesn’t go away with brushing.
- Pus draining from the gums or a “pimple” on the gum.
- Trouble opening your mouth or feeling “locked.”
Gastrointestinal Symptoms
When an infection spreads, it doesn’t just stay in one part of the body; it can also affect the digestive system. These gastrointestinal symptoms might not immediately make you think “tooth infection,” but they’re often linked to systemic inflammation and the body’s immune response:
- Nausea or vomiting, especially when combined with fever and facial swelling.
- Diarrhea or loose stools that appear “out of the blue” but coincide with a worsening toothache.
- Abdominal pain or cramping, sometimes without a clear food or virus cause.
Cardiovascular Symptoms
Once an infection reaches the bloodstream, it can impact the cardiovascular system in serious ways. The symptoms listed below are indicators that the infection may be placing stress on your heart and circulation—conditions that require immediate medical attention:
- Rapid heart rate
- Low blood pressure
- Shortness of breath or fast breathing.
Neurological Symptoms
Though less common, a spreading dental infection can occasionally impact the nervous system. These neurological symptoms may appear in more advanced stages and should never be ignored, as they could point to serious systemic involvement or even infection in the brain:
- Confusion or trouble thinking clearly.
- Seizures
- Numbness or tingling in the face or limbs
Other Symptoms
While these symptoms may not be as common, they can still occur in some cases and are worth being aware of—especially if they appear alongside more classic signs of infection. They may indicate that the infection is taking a toll on other systems in the body:
- Joint pain or stiffness that flares with dental issues.
- Skin rash or itching on the face or neck.
- Unplanned weight loss over weeks, especially with fatigue and repeated tooth problems.

When Is a Tooth Infection an Emergency?
Not all tooth infection symptoms require emergency care, but some signs indicate that the infection may be spreading and needs immediate medical attention. You should seek urgent dental care if you experience:
- Swelling in the face or neck that is rapidly worsening, especially if it begins to affect your ability to open your mouth or move your jaw
- Difficulty breathing or swallowing, which may indicate airway obstruction from swelling in the jaw or throat
- High fever (above 101°F / 38.3°C) or persistent chills, signaling that the infection may be spreading systemically
- Confusion, dizziness, or unusual drowsiness, which can be signs of severe infection or early sepsis
- Severe, throbbing pain combined with swelling or fever, especially if it does not improve with over-the-counter pain relief
Causes and Risk Factors of Dental Infections
Understanding what causes a dental infection and who is more likely to develop one is key to preventing serious complications. Several factors can increase your risk, from everyday habits to underlying health conditions. Here are some of the most common causes and risk factors that could set the stage for an infection:
- Poor Oral Hygiene: Not brushing or flossing regularly allows plaque and bacteria to build up, increasing the risk of cavities and infections.
- Bacterial Invasion: Bacteria can enter the tooth through cracks, cavities, or gum pockets, leading to inflammation and infection.
- Tooth Decay: Advanced decay can penetrate the enamel and reach the pulp, where infection can take root and spread.
- Trauma: Cracks or chips from injuries can expose the tooth’s inner tissues to bacteria.
- Wisdom Teeth: Impacted or partially erupted wisdom teeth are prone to infection due to difficulty cleaning them properly.
- Weakened Immune System: Conditions like diabetes or autoimmune diseases can impair the body’s ability to fight off infection.
- Smoking: Tobacco use weakens the immune system and damages gum tissue, making infections more likely and harder to treat.
- Bad Diet: Diets high in sugar and low in essential nutrients can feed harmful bacteria and impair the body’s defenses.
Complications of an Untreated Dental Abscess
Ignoring a dental abscess can have far-reaching consequences beyond tooth loss. When bacteria from an untreated infection spread, they can affect vital organs and systems, leading to serious, even life-threatening, health conditions. Understanding these complications underscores the importance of seeking treatment early before the infection has a chance to escalate.
Gum Disease
When left untreated, a tooth abscess can contribute to or worsen periodontal disease. This condition affects the gums and supporting structures of the teeth, potentially leading to tooth loss and bone damage. Gum disease also increases the risk of systemic issues, making it more than just a local oral health concern.
Ludwig’s Angina
This rare but serious complication is a type of cellulitis that affects the floor of the mouth and neck. Caused by a spreading dental infection, Ludwig’s angina can lead to difficulty breathing or swallowing and requires emergency treatment to prevent airway obstruction.
Dental Cysts
An untreated abscess can result in the formation of a dental cyst, an enclosed sac filled with fluid or pus near the tooth root. While sometimes harmless, cysts can become infected or grow large enough to cause discomfort, damage to the jawbone, or displacement of nearby teeth.
Sepsis
Sepsis is a life-threatening reaction to infection that occurs when the body’s immune response causes widespread inflammation. A dental abscess that enters the bloodstream can trigger this dangerous condition, leading to organ failure or death if not treated promptly in a hospital setting.
Osteomyelitis
Osteomyelitis is a serious bone infection that can result from bacteria spreading from a dental abscess. It most commonly affects the jaw and can lead to persistent pain, swelling, and destruction of bone tissue. Treatment often requires antibiotics and, in some cases, surgical intervention.
Endocarditis
Endocarditis is an infection of the inner lining of the heart chambers and valves, often caused when bacteria from a dental infection enter the bloodstream. People with preexisting heart conditions are especially at risk. This complication can be life-threatening and demands immediate medical care.
Before & After Photos
* All patients are unique and individual results may vary.
Available Treatments for a Dental Abscess
Treating a dental abscess requires swift and targeted intervention to eliminate the infection and prevent further complications. Depending on the severity and spread of the infection, treatment may involve medication, surgical procedures, or both. Below are some of the most common and effective approaches used by dental professionals today.
Antibiotics
Antibiotics are often the first line of defense when treating a dental abscess, especially if the infection has started to spread. They help eliminate the bacterial infection and reduce inflammation. While they won’t fix the root problem, antibiotics are essential for stabilizing the patient before any further dental procedures.
Apicoectomy
An apicoectomy is a surgical procedure used when a standard root canal isn’t enough to remove the infection. It involves removing the tip of the tooth’s root and sealing it to prevent reinfection. This treatment is often recommended when an abscess persists after previous endodontic therapy.
Drainage
In some cases, draining the abscess is necessary to relieve pressure and remove pus from the infected area. This procedure is typically performed under local anesthesia and provides immediate relief from pain. Drainage is often combined with antibiotics and other dental treatments to fully resolve the infection and prevent recurrence.
Treatment of sepsis
When a dental infection progresses to sepsis, it becomes a medical emergency. Treatment typically involves hospitalization, intravenous antibiotics, and supportive care to stabilize blood pressure and organ function. Prompt intervention is critical, as sepsis can escalate rapidly and result in serious long-term consequences or death if not addressed immediately.
Root canal treatment
Root canal therapy is a common and effective way to treat a dental abscess when the infection is confined to the tooth. During this procedure, the infected pulp is removed, the inside of the tooth is cleaned and sealed, and a crown is usually placed for protection. It saves the natural tooth and prevents future infections.
Why Choose Dr. Gallardo in Miami, FL?
Treating a dental abscess isn’t just about relieving pain; it’s about preventing long-term complications. That’s why it’s so important to trust your care to a seasoned professional. An experienced dentist understands how to identify the earliest signs of a spreading infection and provide targeted treatment to protect your overall oral health.
At Gallardo Periodontics and Implant Dentistry, Dr. John Paul Gallardo, DDS, PA, is a highly experienced periodontist with more than 30 years of specialized practice focused on gum disease and dental implants. He received advanced training from institutions such as the University of Miami, New York University College of Dentistry, and Boston University, and has lectured nationally and internationally on periodontal and implant-related treatments.
Dr. Gallardo also serves as a clinical educator and has treated thousands of patients, performing hundreds of procedures each year using advanced diagnostic techniques and modern treatment approaches.
Call us today at 305-447-1447 or visit our contact page to schedule your consultation.
Frequently Asked Questions About Tooth Infections
Can you get sepsis from a tooth infection?
Yes, a tooth infection can lead to sepsis if bacteria enter the bloodstream and trigger a widespread inflammatory response. Sepsis is a life-threatening condition that requires immediate medical treatment. Warning signs include high fever, rapid heart rate, confusion, and low blood pressure.
Can an infected tooth make you sick?
Yes, especially if the infection begins to spread. Common symptoms include fever, fatigue, nausea, and a general feeling of illness. As bacteria enter the bloodstream, the body may respond with flu-like symptoms, which is often a sign that the infection is no longer localized.
How long can a tooth infection go untreated?
A tooth infection can worsen within days or weeks, depending on the severity and your overall health. While symptoms may improve, the infection does not go away on its own and can continue spreading silently. It can eventually lead to serious complications if left untreated.