
Have you recently had a tooth extraction and now feel a sharp, throbbing pain that won’t go away? You might be experiencing a dry socket, one of the most uncomfortable complications that can occur after dental surgery.
Though painful, a dry socket is treatable and preventable with the right care. In this post, we’ll explain exactly what a dry socket is, how to treat it, and what steps you can take to ensure a smooth and speedy recovery. Keep reading to learn how to ease the pain and protect your smile.
What is a Dry Socket?
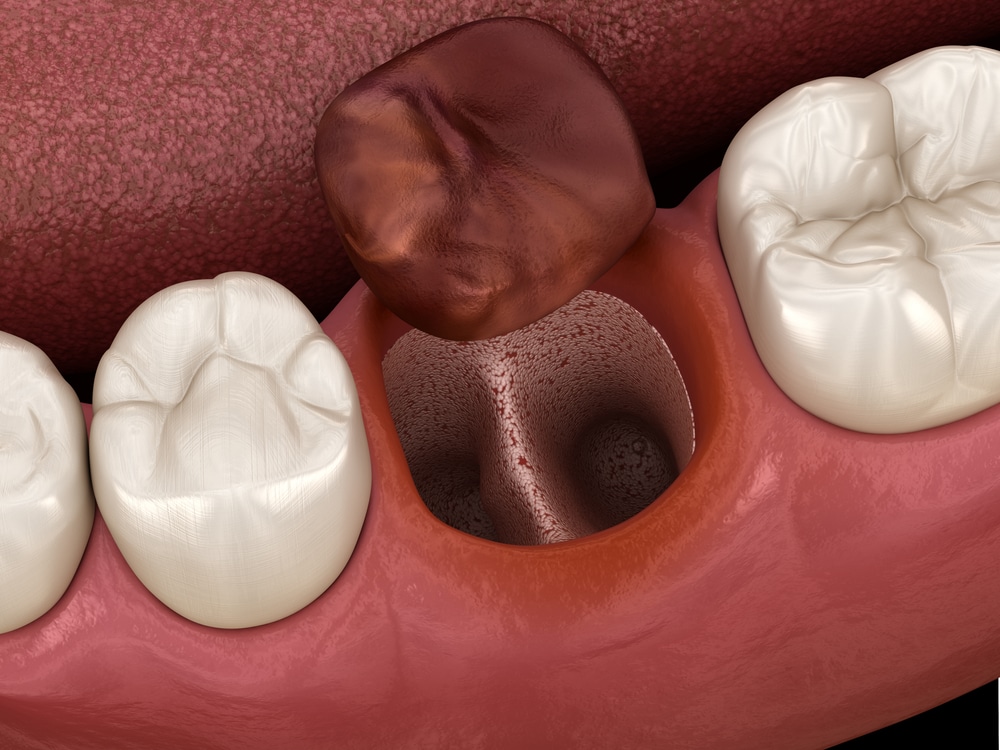
A dry socket, or alveolar osteitis, is a painful dental condition that can occur after a tooth is extracted, especially wisdom teeth. Normally, a blood clot forms at the site to protect the bone and nerves underneath. But if that clot dissolves or becomes dislodged, the bone is exposed—causing intense pain. Dry sockets typically develop 2-5 days after extraction and require professional care. Let’s explore what you need to know to handle this condition effectively.
Is Dry Socket Dangerous?
While dry sockets can be quite painful, they rarely result in serious complications or infections. However, they can delay the normal healing process after a tooth extraction. In some cases, the discomfort may linger longer than expected, and if left untreated, a dry socket can increase the risk of developing an infection in the area.
How to Treat a Dry Socket With a Professional
Professional care is often the fastest and most reliable way to relieve dry socket pain and jumpstart healing. Dentists have the tools and expertise to manage the condition directly at the source, offering both immediate relief and long-term protection. Here are the most common in-office dry socket treatments you can expect during a visit:
1. Professional Cleaning
The first step a dentist takes to treat a dry socket is carefully cleaning the affected area. This involves flushing out any trapped food particles or debris to reduce the risk of infection. Cleaning also helps prepare the site for further treatment and allows the healing process to begin properly.
2. Medicated Dressing
After cleaning, the dentist will place a medicated dressing into the dry socket. This special gauze is soaked with soothing medication that helps reduce pain and protect the exposed bone. The dressing also encourages new tissue to form, promoting faster healing. It may be replaced every few days as needed.
3. Pain Relief Medication
To help manage discomfort, your dentist or doctor may recommend over-the-counter or prescription pain relievers. These medications are tailored to your pain level and medical history. Proper pain control allows you to stay comfortable while the area heals, and it’s especially helpful in the first few days after treatment begins.
4. Antibiotics
Antibiotics are not always necessary for dry sockets, but your dentist may prescribe them if signs of infection appear. Symptoms like swelling, pus, fever, or persistent bad breath may indicate a deeper issue. In these cases, antibiotics help eliminate harmful bacteria and support your body’s natural healing process.
Dry Socket Home Remedies
While professional treatment is the best route for managing dry sockets, there are also home remedies that can help ease discomfort while your mouth heals. These natural options are not a replacement for a dentist’s care but may provide temporary relief when used safely and as part of a comprehensive care plan.
Warm Salt Water Rinse
A gentle warm rinse with salt water can help clean the affected area and support healing. Mix 1/2 teaspoon of salt into 8 ounces of warm water and swish it around your mouth for 30–60 seconds. Do this several times a day to reduce inflammation and lower the risk of infection.
Cold and Warm Compresses
Alternating between cold and warm compresses can soothe discomfort and reduce swelling from dry sockets. Apply a cold compress to your cheek for 20 minutes, then follow with a warm compress for another 20 minutes. This combination helps numb the pain while boosting circulation to promote healing in the affected area.
Honey
Raw honey offers natural antibacterial, anti-inflammatory, and pain-relieving benefits. To use it, soak a sterile gauze pad in honey and gently place it over the dry socket. This can help reduce pain and protect the area from infection. Change the dressing every few hours for continued relief and cleanliness.
Tea Tree or Clove Oil
Clove oil is known for its natural anesthetic properties and can bring quick relief. Apply a small amount to clean gauze and place it over the socket for temporary pain relief. Tea tree oil, a natural antiseptic, may be diluted and combined with honey or black tea before gentle application with sterile gauze.
Black Tea Bags
Black tea contains tannins, which are natural compounds that help reduce inflammation and fight bacteria. Soak a tea bag in warm water, let it cool slightly, then gently place it on the dry socket. This method can ease discomfort while creating a mild antibacterial barrier that supports the healing process.

Tips for Faster Mouth Healing From Dry Socket
To recover more quickly from dry socket, it’s important to support your body’s natural healing process with the right habits. These simple tips can help reduce discomfort, protect the socket, and speed up recovery time—while lowering the risk of further irritation or complications.
- Don’t smoke, use tobacco, or drink alcohol
- Avoid using straws for one week after your extraction
- Avoid strenuous physical activities for a few days
- Avoid chewing on the affected side and consuming hot or irritating foods and beverages
- Drink plenty of clear fluids
When Should I See a Dentist for a Dry Socket?
If you’re feeling sharp pain days after your tooth extraction—or if the discomfort seems to get worse instead of better—it’s time to call your dentist. Other red flags include a foul taste or odor in your mouth and pain that doesn’t ease with medication. Prompt care prevents complications and speeds up healing.
Get Dry Socket Diagnosis and Treatment from a Professional
When it comes to dry sockets, timing and experience matter. Treating it promptly helps minimize pain and prevent complications like infection or prolonged healing. An experienced dental professional can clean the area, protect the exposed bone, and support your healing for the best results.
With over 25 years of experience in periodontics and implant dentistry, Dr. John Paul Gallardo has helped countless patients recover comfortably from dry sockets and other post-extraction complications. At Gallardo Periodontics and Implant Dentistry, our advanced dental clinic and sedation options make your visit stress-free and effective. Call us at 305-447-1447 or visit our contact page to schedule a consultation.
Frequently Asked Questions
When can I stop worrying about dry socket?
You can generally stop worrying about dry sockets about 7 to 10 days after a tooth extraction. By this time, the gum tissue usually heals enough to protect the area. Still, everyone’s healing process is different, so it’s crucial to follow your dentist’s instructions and report any unusual pain, swelling, or other dry socket symptoms right away.
What are the symptoms of dry socket?
Dry socket is one of the most painful complications that can occur after a tooth extraction. It typically develops when the blood clot at the extraction site becomes dislodged or dissolves too early, exposing the bone and nerves underneath. This leads to an empty socket, which causes severe pain that often radiates to the ear, eye, or neck on the same side as the extraction. Patients may also notice a bad taste or odor coming from the mouth. Unlike typical post-extraction discomfort, dry socket pain usually starts a few days after the procedure and worsens over time. The surrounding teeth and gums may become sensitive and inflamed, requiring prompt treatment by a dental professional.
How to avoid dry socket after a wisdom teeth extraction?
To avoid dry socket after wisdom teeth removal, it’s essential to follow your dentist’s post-operative instructions carefully. One of the most common complications following a difficult tooth extraction is dry socket, which can be extremely painful. To reduce the risk, avoid smoking, drinking through straws, or spitting forcefully, as these actions can dislodge the blood clot that forms in the socket. Maintaining good oral hygiene is also important, but be gentle—avoid brushing directly over the wisdom tooth extraction site for the first couple of days.
Certain risk factors—such as smoking, previous dry sockets, and poor oral care—can increase your chances of developing this condition. Staying hydrated, eating soft foods, and attending follow-up appointments can further help you heal properly and prevent complications.